CO₂ Tolerance and the Bohr Effect: Why Slower Breathing Might Be Your Body’s Secret Weapon for Better Oxygen Delivery
We’ve all heard the advice: breathe deep, pull in more oxygen, and feel better. But what if the real key isn’t flooding your lungs with air? What if it’s learning to comfortably hold onto a bit more carbon dioxide?
The Bohr Effect: CO₂ as Oxygen’s Smart Delivery Partner
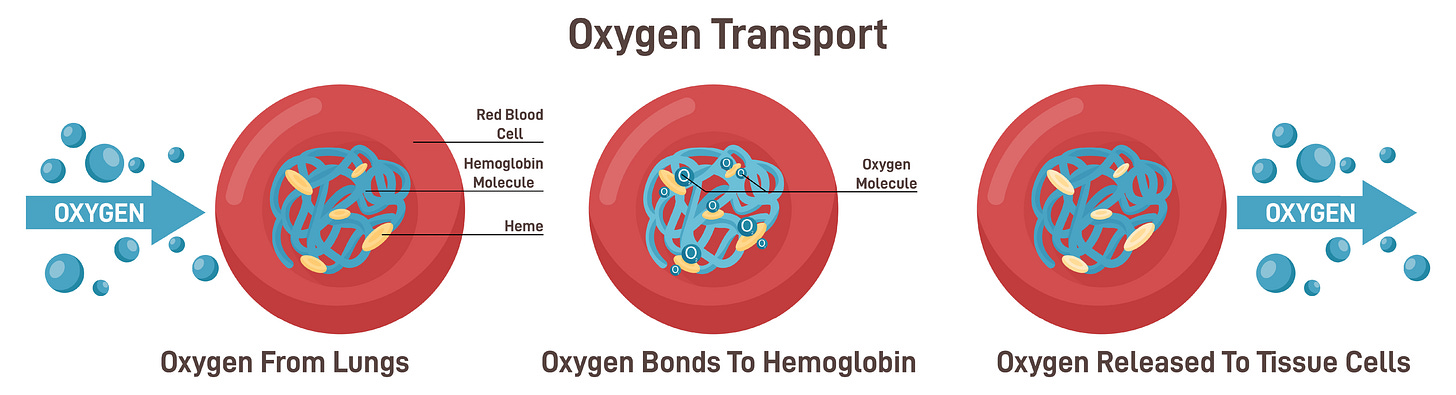
Back in 1904, Danish physiologist Christian Bohr noticed something remarkable. When tissues work hard and produce more CO₂—which naturally lowers local pH—hemoglobin in your red blood cells loosens its grip on oxygen and releases it right where it’s needed most.
It’s as if CO₂ tells hemoglobin, “Hey, drop the oxygen here. These muscles and brain cells are hungry.”
This shift moves the oxygen-hemoglobin dissociation curve to the right. The result? Easier unloading of oxygen in active tissues while the lungs still load it efficiently. Peer-reviewed physiology confirms the effect. Studies show that elevated CO₂ and lower pH enhance delivery to tissues, while low CO₂ from over-breathing makes hemoglobin hold onto oxygen more tightly. Your cells can end up subtly under-oxygenated even when your pulse oximeter reads 98%. Modern modeling reinforces how important this is. When CO₂ levels stay in a healthy, slightly elevated range, the entire oxygen transport system works better.
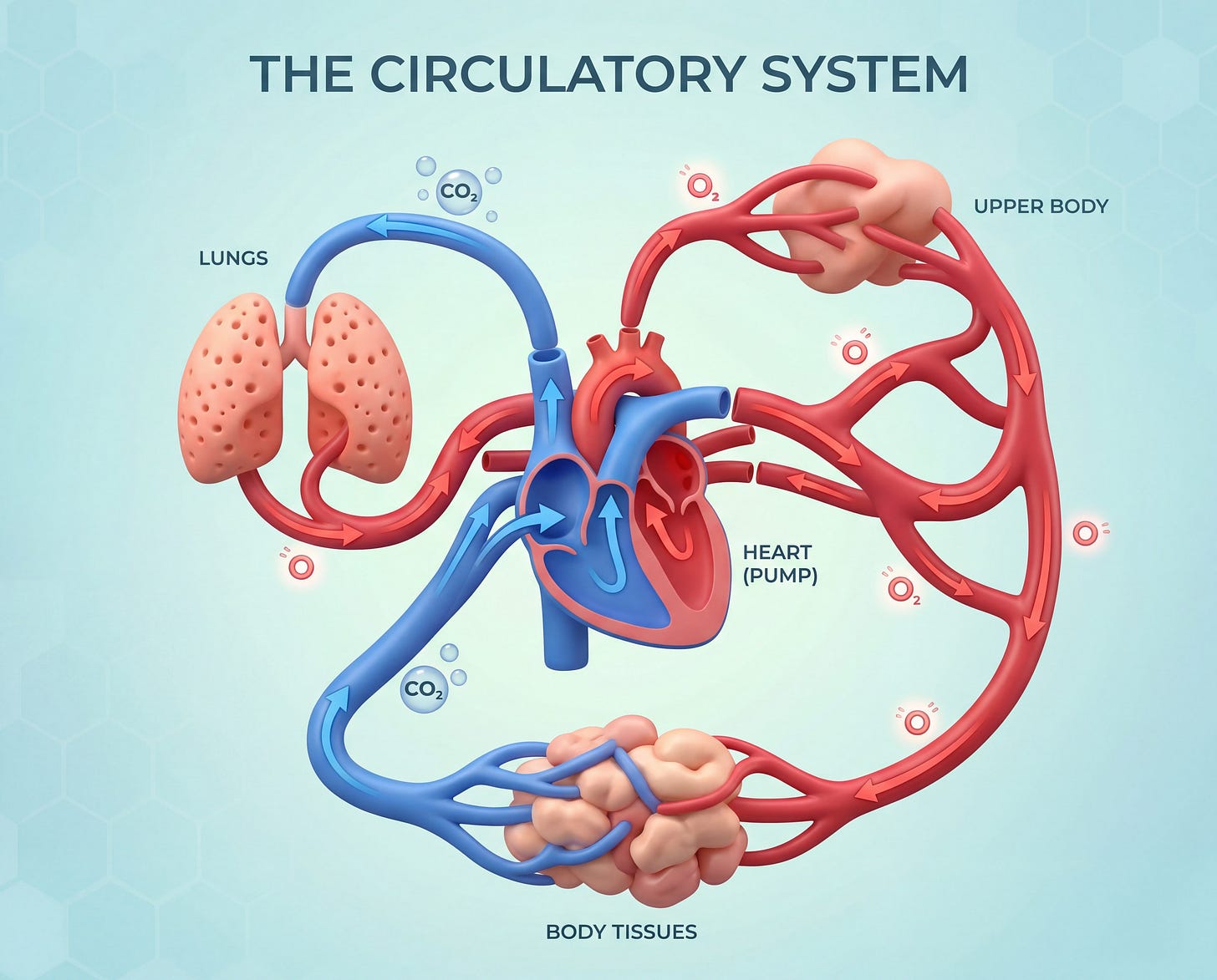
Why Modern Breathing Habits Sabotage This System
Chronic shallow breathing, mouth breathing, and stress-driven rapid breaths blow off too much CO₂. This creates hypocapnia: your blood turns more alkaline, the Bohr effect weakens, and you can feel foggy, fatigued, or anxious even though you’re “getting plenty of air.” Most of us today have lost our natural tolerance for normal rises in CO₂. Our brains sound the alarm and force us to breathe at the slightest increase.
The Benefits of Building CO₂ Tolerance
By practicing slower, nasal, diaphragmatic breathing, you retrain your system to a calmer baseline. Oxygen utilization improves through the Bohr effect. You also gain smoother energy, reduced anxiety from stronger parasympathetic tone, sharper focus, and faster recovery.
Clinical research supports these gains. Slow breathing has been shown to improve blood oxygenation at altitude and enhance outcomes in chronic heart failure patients by increasing baroreflex sensitivity.
Simple Ways to Start Improving Your CO₂ Tolerance
The approach is refreshingly straightforward.
Switch to nasal breathing as much as possible, day and night. Let your exhale last a little longer than your inhale. Add gentle breath holds after exhaling—nothing forced. Over weeks, your body adapts. The Bohr effect works more efficiently, and you start noticing steadier energy and a deeper sense of calm.
Final Thoughts: Breathe Smarter, Not Harder
Science has understood this elegant dance between O₂ and CO₂ for over 120 years. Now it’s time to use it. Breathe a little less volume, tolerate a little more CO₂, and let your tissues thank you with clearer thinking, steadier energy, and greater resilience.
Like what you read? Keep exploring…
If this post resonated with you, you may enjoy my new book:
The Science of Medical Qigong: How Breath, Movement, and Attention Transform the Body
This book examines the growing body of scientific research exploring how Qigong practice influences human physiology. Drawing from clinical trials and experimental studies, it explains how coordinated breathing, posture, movement, and focused attention interact with the body’s regulatory systems.
The book explores research on:
• autonomic nervous system regulation
• cardiovascular function and blood pressure
• respiratory mechanics and lung capacity
• sleep quality and recovery
• inflammatory and immune signaling
• brain function and neural plasticity
• cognitive performance and mental health
Rather than presenting Qigong through mystical language, The Science of Medical Qigong approaches the subject through physiology, neuroscience, and clinical research, offering a clear explanation of how regular practice can influence the coordination and harmony of the body’s systems.
Available now in print and Kindle formats.
Click here to get your copy on Amazon
References
Benner, A., Patel, A. K., & Singh, K. (2023). Physiology, Bohr effect. In StatPearls. StatPearls Publishing.
Bernardi, L., Porta, C., Spicuzza, L., Bellwon, J., Spadacini, G., Frey, A. W., Yeung, L. Y. C., Sanderson, J. E., Pedretti, R., & Somers, V. K. (2002). Slow breathing increases arterial baroreflex sensitivity in patients with chronic heart failure. Circulation, 105(2), 143–145.
Bilo, G., Revera, M., Bussotti, M., Bonacina, D., Styczkiewicz, K., Caldara, G., Giglio, A., Faini, A., Giuliano, A., Lombardi, C., Kawecka-Jaszcz, K., Mancia, G., & Parati, G. (2012). Effects of slow deep breathing at high altitude on oxygen saturation, pulmonary and systemic hemodynamics. PLoS ONE, 7(11), Article e49074.
Malte, H., Lykkeboe, G., & Wang, T. (2021). The magnitude of the Bohr effect profoundly influences the shape and position of the blood oxygen equilibrium curve. Comparative Biochemistry and Physiology Part A: Molecular & Integrative Physiology, 254, Article 110880.
Patel, S., Jose, A., & Mohiuddin, S. S. (2023). Physiology, oxygen transport and carbon dioxide dissociation curve. In StatPearls. StatPearls Publishing.